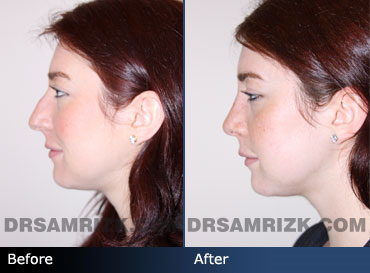
Septoplasty, or deviated septum surgery, does more than just straighten a deviated septum. It can also help with a number of health problems.
A deviated septum — whether congenital, stemming from trauma or the result of a previous rhinoplasty procedure — can contribute to all kinds of health issues, including nasal obstruction, allergy problems, epistaxis (nosebleeds) and obstructive sleep apnea.
Let’s take a look at how these problems come about and how straightening the septum can help.
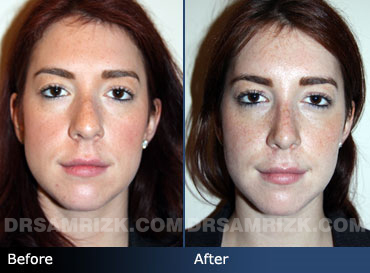
Nasal Obstruction (Breathing)
Many things can cause nasal obstruction, including a deviated septum. If you are experiencing nasal obstruction, your ear, nose and throat specialist will conduct a thorough examination to determine what is impeding your nasal airway and how to treat it.
Septoplasty is not always required to clear the nasal airway. If, for example, your doctor suspects swelling from allergies to be the cause, he or she will likely begin your course of treatment by ordering allergy tests. If it turns out that allergies are causing the problem, your doctor may prescribe you antihistamines or nasal steroid spray, which shrink the nasal tissue and open the airway. Other patients may require a procedure to reduce the size of the turbinates, or a functional endoscopic sinus surgery (FESS) to drain the sinuses. Still others require a functional rhinoplasty procedure, possibly including spreader grafts if internal valve narrowing is involved.
If, however, your doctor determines that a deviated septum is to blame for your nasal obstruction, he or she may recommend that you undergo septoplasty to straighten your septum and restore proper breathing. (Nasal obstruction due to a deviated septum is defined as obstruction of 50 percent or more.) In some cases, it may be necessary to perform septoplasty in combination with rhinoplasty and/or sinus surgery.
Allergies
Allergies can cause swelling of the turbinates and other internal structures within the nose, resulting in blockage of the nasal airway. This can be a real problem if you have a deviated septum, as your septum may already by causing some blockage. Luckily, your ear, nose and throat specialist can employ a number of strategies to clear up your airway and improve breathing. This may include antihistamines, nasal steroid spray, endoscopic sinus surgery, spreader grafts for internal valve narrowing, and of course, septoplasty if you have a deviated septum.
Epistaxis (Nosebleeds)
Nose bleeds (epitastaxis) can be caused by a variety of things, including a deviated septum. In a straight nose, air enters the nose without causing any turbulence, in turn allowing for normal breathing. In a person with a deviated septum, turbulence may be created when air hits the curve of the septum, which causes the septum’s lining to dry out and begin cracking. This also increases vascularity in the area, which increases the risk of nosebleeds.
If a deviated septum is to blame for your nosebleeds, straightening the septum through septoplasty will likely be the appropriate treatment. Septoplasty can eliminate the unnatural curvature of a deviated septum, thereby reducing turbulence and the process it sets in motion that eventually leads to nosebleeds.
Obstructive Sleep Apnea
If left untreated, a deviated septum can cause obstructive sleep apnea, a potentially dangerous condition that must be addressed. Obstructive sleep apnea is characterized by shallow breathing. One symptom of the condition is snoring. Those suffering from obstructive sleep apnea wake up frequently during sleep, and usually do not remember it. Sleep apnea keeps the body from going into deep sleep, resulting in sleep deprivation and fatigue during the day.
Straightening the septum through septoplasty can restore the airway and improve breathing, which helps to address sleep apnea.
The Procedure
Surgery to repair a deviated septum takes one to two hours and is performed under general anesthesia.
Dr. Rizk uses a 3D telescope to view the septum and other internal nasal structures during the surgery. This and other advanced techniques and instruments allow him to make minimal alterations, for a better outcome and shorter recovery.
During septoplasty, Dr. Rizk lifts and separates the mucus membrane covering the septum. Straightening the septum involves removing portions of cartilage and bone that are blocking airflow. Next, Dr. Rizk returns the membrane to its original position and uses stitches or tissue glue to seal any wounds. He may place internal splints, which will be removed a few days later. Septoplasty patients remain at the clinic for a few hours before returning home.
If performed alone, i.e., not in combination with rhinoplasty or another procedure, septoplasty usually does not lead to a lot of swelling and bruising. However, congestion and slightly compromised nasal breathing are common for a few weeks following surgery.
Dr. Rizk provides his septoplasty patients with comprehensive postoperative instructions. It is important to follow these instructions closely. You will not be able to participate in strenuous activities for at least a week, and will need to avoid contact sports for a period of months or even up to one year (until such time as the nose has fully healed). However, you should be back to your normal routine in a few days. Over-the-counter pain medications should suffice for any discomfort you experience. The splints will be removed about a week after the surgery.
To learn more about the benefits of septoplasty, contact Dr. Rizk’s office today.