In general, patients seeking revision rhinoplasty and those considering rhinoplasty for the first time have different complaints they would like to address. This document discusses the different complaints as well as how they may be addressed by a facial plastic surgeon.
Primary Rhinoplasty: The Most Common Complaints
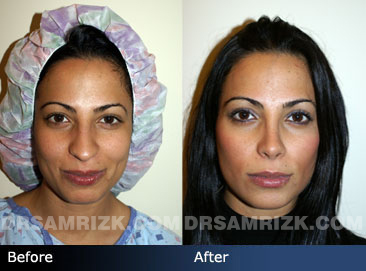
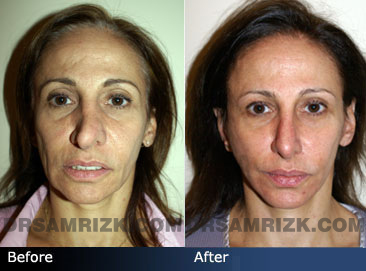
Patients considering rhinoplasty for the first time often want their nose to be smaller or have a more refined appearance. The two most common complaints among this patient group are a) a nose that’s too large and b) a nasal bump(s). Let’s discuss these common complaints and how they are treated.
A Large Nose
For patients who feel that their nose is too large, the good news is that many physical characteristics of a large nose can be improved, refined and reduced, including projection of the nose, wide nasal bones and thick upper lateral and lower lateral cartilages. As with any surgical procedure, there are limitations.
Any number of rhinoplasty techniques may be used to reduce the size of a large nose and improve its appearance. It all depends on the patient’s unique nasal structure. The goal is to reduce the size of the nose while maintaining harmony with the rest of the face. Computer imaging is often useful when planning such a procedure. Reducing the size of the nose often requires osteotomies and techniques to refine a large tip, such as alarplasty, as well as the removal of a dorsal hump.
Nasal Bumps
The other highly common complaint among first-time rhinoplasty patients is nasal bumps. Nasal bumps are often congenital but are also a common result of trauma to the nose. A nose injury may flatten part of the nose, in turn creating a bump. There are many things that can cause a nasal bump, so, as with any rhinoplasty procedure, surgery to correct a nasal bump is always tailored to the individual patient.
If the bump is large, the nasal bones may need to be “infractured” and then brought together, to eliminate the possibility of an issue called open roof deformity. If the bump is caused by excess cartilage, it can be shaved down. If the bump is due to a depression between the eyes, it may be possible to insert a graft in the area to fill the depression. Or, if the bump is in the lower third of the nose and came about as a result of trauma that caused the septum to lower, the septum can be raised. Drooping due to aging can also lead to nasal bumps.
Again, there are many possible causes, so you will need to schedule a consultation with Dr. Rizk to find out exactly what is causing your nasal bump(s). Dr. Rizk will view the bump with a 3D camera to determine what is causing the problem, prior to determining the best course of action in your case.
Revision Rhinoplasty: The Most Common Complaints
The complaints that facial plastic surgeons hear from patients wishing to have revision rhinoplasty are more varied than those from primary rhinoplasty patients. As a result, the techniques used to address the complaints of revision rhinoplasty patients are also more varied. It all depends on which part(s) of the nose needs correction.
A Crooked Nose
That being said, the most common complaint among revision rhinoplasty patients is a crooked nose. Addressing this may require straightening all three of the major nasal structures:
- The bony bridge
- The cartilage bridge
- The tip cartilage
If the bones are pushed to one side, osteotomies, or controlled breaks, will likely be necessary to realign the bones. If the septum or other cartilage is deviated, suturing techniques will probably be used. Spreader grafts are often used in the middle section of the nose to align the midline and teeth, for symmetry. If the septum is fractured, it is most likely twisted and will therefore need to be straightened; straightening the septum is also important for breathing.
If your nose is fractured, you may need to wait for a matter of months before receiving treatment.
Dr. Rizk usually makes small internal incisions to access the deviated, obstructive or damaged tissue. He utilizes 3D imaging technology to view the tissues. This enables him to minimize trauma to the tissues, in turn reducing recovery time. Small instruments are used to alter or manipulate the tissues.
Straightening a crooked nose is a very challenging endeavor that requires the experience of a board-certified facial plastic surgeon specializing in rhinoplasty.
Mucous Cyst Formation
The formation of a mucous cyst after rhinoplasty is exceedingly rare and should be considered a late soft tissue complication of septorhinoplasty. To Dr. Rizk’s knowledge, fewer than 10 cases have been reported in world literature to date. In all previous cases, the mucous cyst appeared several months to years after rhinoplasty. Sites described include the glabellar region and the bony and cartilaginous nasal dorsum, as well as the area overlying the alar cartilages.
On exploration, a distinct capsule with no direct connection between the nasal mucosa and the cyst was reported in all cases. The most reasonable explanation for this phenomenon appears to be the proliferation of ectopic or displaced mucous membranes, acting as free grafts, caused by the improper clearing of mucous epithelial remnants attached to bone or cartilage either in situ or as part of an autogenous graft. It is also hypothesized that cysts may develop by occlusion of sebaceous glands because of scar tissue formation.10 In our case, the cyst undoubtedly formed as a result of an incomplete osteotomy, with superior displacement and sequestration of the nasal bone and its attached mucous remnant.
Post Rhinoplasty nasal-dorsal mucous cyst formation is a preventable complication. Meticulous removal of all bony, cartilaginous, and mucous remnants is essential. Maintaining mucosal integrity during intranasal osteotomy and completing all osteotomies are also important to prevent such post-rhinoplasty complications as mucous cysts. Treatment of this unfortunate complication is complete excision through an intranasal or open approach. Read the detailed report of a case of an expanding nasal-dorsal mucous cyst that developed after a closed septorhinoplasty procedure in a 33-year-old male, published by Romo T 3rd, Rizk SS, Suh GD.
Other Complaints Commonly Addressed by Revision Rhinoplasty
- Retracted Nostrils
Also called alar retraction because it involves a retraction of the alar cartilages, retracted nostrils often arise after an aggressive primary rhinoplasty procedure. Alar retraction occurs when part of the ala contracts upward, which leaves too much nostril showing. Though this condition can also be congenital when resulting from a primary rhinoplasty procedure it typically occurs because too much cartilage was excised — or not enough. Grafting with alar batten grafts, alar rim grafts, and/or composite grafts may be required, and the cartilage will likely need to be repositioned. - Pinched Tip
A pinched tip is a nasal tip that looks too narrow or “pinched.” It can be congenital or may result from over-resection of the tip cartilages during a primary rhinoplasty procedure. A pinched tip is addressed through a procedure called “tip-plasty,” which reshapes the tip with ear or other cartilage. Grafting with alar batten grafts may be performed. - Dorsal Scoop
Also known as a saddle nose deformity or “scooped nose,” a dorsal scoop is a saddle-like formation in the area of the septum. It occurs when something causes the septum to lower, such as trauma. To correct this issue, a procedure is performed to raise the septum. -
Hanging Columella
The columella is the strip of skin between the nostrils. A hanging columella (sometimes called alar-columellar disproportion) is one that hangs lower than the desired position, so that around 4mm of nostril is visible from the profile. A hanging columella can have many possible causes. Sometimes it is congenital, in which case it is often caused by a long septum that pushes down on the columella.In other cases, it is the result of a mistake made during a primary rhinoplasty procedure. To address it, excess tissue may be excised and a section of the septum may be removed. Other cartilage may be removed or shaved as well. In rare cases, the nasal spine is reduced.
- Short Nose
A short nose is one that is too short in proportion with the rest of a person’s face. In many cases, it involves an upturned, over-rotated tip. To correct this, the scar from the original rhinoplasty procedure will likely need to be released so that the tip can be moved to a less-rotated position. Several cartilage grafting techniques may be used to create sufficient support, including caudal septal extension grafting and extended spreader grafts.A short nose can also be caused by a low radix, in which case radix grafting can be used to raise the bridge in the area in question. A short nose is one of the most challenging issues to address in rhinoplasty. The key is to create sufficient support to sustain the nasal tip in its new position.
- Pointy Tip
A pointy tip occurs when the alar cartilages are too prominent, i.e., they appear too pointy or stick out too much. This can be the result of genetics (usually in thin-skinned individuals) or may be a result of the original rhinoplasty procedure. To address a pointy tip, cartilages may be shaved or trimmed and fascia or a soft tissue graft may be placed over the tip cartilages.
To learn more about common complaints among primary rhinoplasty and revision rhinoplasty patients, please contact Dr. Rizk’s office today.